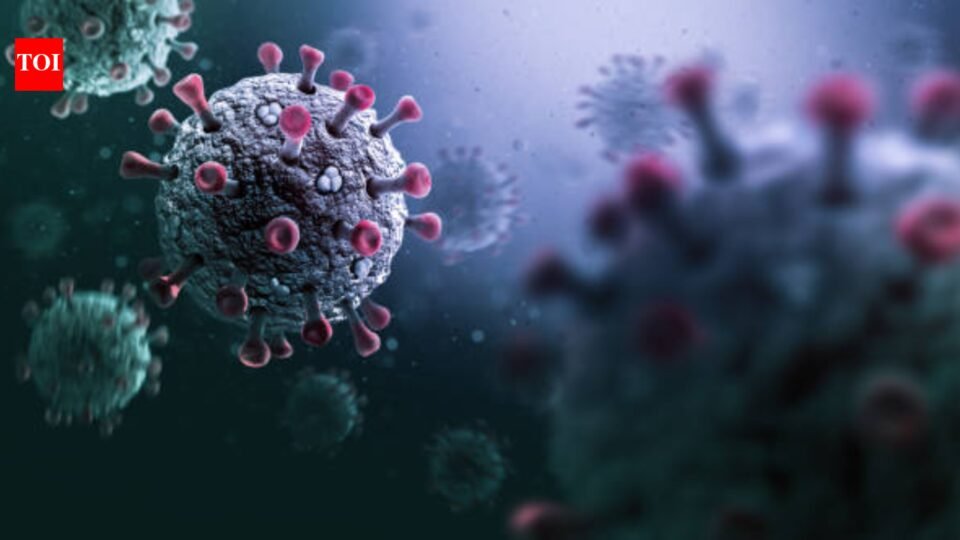
Just when it felt like COVID had quietly slipped into the background of everyday life, a new variant is back in the headlines. Reports suggest this strain carries multiple spike protein mutations and shows signs of immune escape, meaning it may partially dodge the protection built from vaccines or past infections. “First identified in a respiratory sample in South Africa in November 2024, the strain has roughly 70 to 75 substitutions and deletions in the gene sequence of its spike protein relative to the JN.1 variant and its descendant, LP.8.1, the antigens used in the latest COVID-19 vaccines,” a report by CIDRAP, University of Minnesota says. And naturally, that raises a familiar question, are we heading toward another crisis?But doctors say the situation today looks very different from what the world faced a few years ago. There’s caution, yes. But there’s also context. And that context matters.
A virus that isn’t going away
If the past few years have taught us anything, it’s that SARS-CoV-2 isn’t static. It keeps changing. That’s how viruses behave. And this new variant is just another step in that ongoing evolution.Dr. S M Fayaz, Lead & Senior Consultant – Internal Medicine at KIMS Hospitals Bengaluru, puts it simply: “The evolution of SARS-CoV-2 continues to occur and the recent discovery of another variant of this virus to have multiple spike protein mutations clearly demonstrates that COVID-19 is now an endemic respiratory virus that will change over time.”That word—endemic—changes how we should think about COVID now. It means the virus is here to stay, much like the flu. It may surge, settle, and return in cycles. But it’s no longer an unknown threat catching the world off guard.And that’s a big shift from where we started.
Are we looking at another crisis?
It’s an understandable fear. The memory of overwhelmed hospitals and sudden lockdowns isn’t that distant. So when a new variant appears, concern is almost automatic.But Dr. Fayaz urges people to step back and look at the bigger picture. “However, just because a variant has emerged does not mean there is now another crisis as happened at the start of the pandemic.”And there are solid reasons behind that reassurance. For one, a large part of the population now has what doctors call hybrid immunity. That comes from a mix of vaccination and prior infection. It doesn’t make people completely immune, but it does help reduce the severity of illness.
“Depending on vaccines and prior COVID-19 infections, a considerable number of people will have hybrid immunity,” he explains. “Additionally, the healthcare systems are much better prepared to handle respiratory outbreaks with improved access to testing, treatment protocols and antiviral therapies.”So while infections may rise at times, the impact isn’t expected to mirror the early waves of the pandemic.
What immune escape really means
The phrase “immune escape” can sound alarming. But what it actually suggests is that the virus has found ways to partially bypass the body’s existing defenses. That can lead to reinfections or breakthrough cases.Dr. Fayaz breaks it down clearly: “The primary health-related consequence of this new spread is that its capacity to partially evade immunization can lead to an increase in new infections and multiple instances of reinfection.”So yes, people who’ve already had COVID or are vaccinated might still get infected again. That’s not new anymore. Many have already experienced it over the past couple of years.But there’s a difference between getting infected and getting severely ill.
What illness might look like now
For most people, especially those who are otherwise healthy, the pattern of illness isn’t expected to be drastically different from recent Omicron waves.“Although it remains possible that both illness levels, such as mild to moderate degree of illness caused by the new variant, resemble levels of illness we have experienced over the most recent wave of the Omicron variant,” Dr. Fayaz says.That usually means symptoms like fever, cough, fatigue, and general weakness. Unpleasant, yes. But often manageable at home for many.He adds, “Symptoms of recent waves of Omicron includes fever/cough/fatigue, and other symptoms that produce the appearance of still being able to respire adequately while ill—reassuringly most pertain to healthy populations… and they can expect a full year of functional health.”That reassurance matters. Because it reminds us that infection doesn’t automatically mean severe disease anymore, at least for a large section of the population.
The groups that still need to be careful
Even with all the progress, not everyone carries the same level of risk. And this is where the conversation becomes more serious.“The most significant concern continues to fall within certain higher-risk populations; mainly the elderly populations, people with preexisting disease conditions, pregnant women, and patients that can initiate an immune response from their medications,” Dr. Fayaz explains.For these groups, even a milder-seeming variant can lead to complications. Hospitalisation risk remains higher. Recovery can be slower.And that’s why public health messaging continues to focus on protecting the vulnerable, not just tracking case numbers.
Why surveillance still matters
It’s tempting to tune out COVID updates altogether. Many people already have. But experts say that would be a mistake.Tracking variants, monitoring trends, and staying prepared still play a crucial role in preventing sudden escalations.Dr. Fayaz puts it plainly: “The new findings imply the need to maintain genomic surveillance and readiness, not panic.”That balance—between awareness and anxiety—is what health systems are trying to maintain. Because reacting too late can be costly, but overreacting can also create unnecessary fear.
Living with COVID, not fearing it
At this point, COVID behaves more like other seasonal respiratory infections. It may surge during certain times of the year, especially in colder months, and then settle down.“COVID-19 case surges may occur episodically, similar to flu viruses,” Dr. Fayaz says.And that comparison helps. Because it frames the virus as something manageable, not something entirely unpredictable.But living with COVID doesn’t mean ignoring it.
The role of vaccines and simple precautions
Vaccination still remains one of the most effective tools. Especially for high-risk groups, booster doses can make a real difference in preventing severe outcomes.“Although COVID-19 continues to demonstrate characteristically how seasonal respiratory illnesses may present, it is nevertheless crucial that we obtain regular booster vaccinations, get tested promptly, and strongly support the needs of the vulnerable community,” Dr. Fayaz emphasizes.And while many people have moved on from masks and distancing, basic precautions still have their place. Especially during spikes.The virus hasn’t disappeared. It’s just changed form, and so has our response. We’re better equipped now, both medically and mentally. But that doesn’t mean we can afford to ignore warning signs.Medical experts consulted This article includes expert inputs shared with TOI Health by: Dr. S M Fayaz, Lead & Senior Consultant – Internal Medicine at KIMS Hospitals BengaluruInputs were used to explain the nature of the new COVID variant that has undergone 75 mutations.